Several factors may contribute to the development of hip osteoarthritis. In some individuals, previous injuries to the hip joint play a role. A fracture involving the bones of the hip can change the alignment of the joint. When the joint surfaces are no longer perfectly aligned, uneven stress can occur during movement.
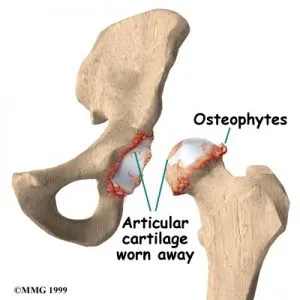
This type of imbalance may lead to increased wear on the cartilage over time. Cartilage damage, infections within the joint, or bleeding inside the joint can also affect the joint surface and contribute to degenerative changes.
Not every case of hip osteoarthritis is related to trauma or joint alignment problems. Genetic factors are believed to influence the likelihood of developing osteoarthritis. Some individuals may inherit structural or biochemical characteristics that make their cartilage more vulnerable to degeneration.
Changes in the subchondral bone may also play a role in the development of osteoarthritis. If the bone beneath the cartilage becomes either too dense or too weak, the way the joint absorbs force can change. This may alter how stress is distributed across the cartilage and lead to gradual deterioration.
Another condition that may lead to hip osteoarthritis is avascular necrosis. In this condition, the blood supply to the femoral head becomes disrupted, causing bone tissue to weaken and collapse. As the shape of the femoral head changes, the joint surfaces no longer align properly, which accelerates degeneration within the hip joint.