Nonsurgical Treatment
Most cases respond well to conservative care. Rest is essential to allow healing and reduce inflammation. Activities that triggered the condition should be temporarily reduced or avoided.
Ice therapy and anti-inflammatory medications help manage pain and swelling in the early stages. Supportive taping techniques may be used to reduce strain on affected tissues, though they are intended to assist healing rather than allow continued overuse.
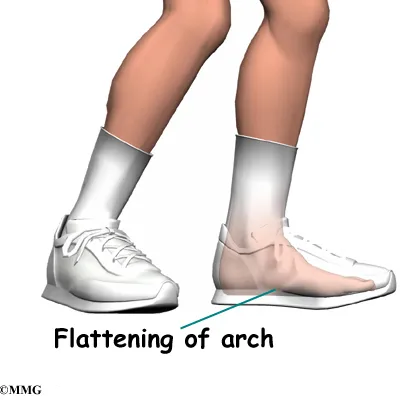
Shock-absorbing insoles or orthotics may be recommended, particularly for individuals with flat arches or alignment issues.
Working with a physical therapist can be highly beneficial. Therapy focuses on reducing inflammation, correcting movement patterns, and addressing the underlying causes of the condition. Guidance on proper footwear, training adjustments, and running technique helps prevent recurrence.
In rare cases, cortisone injections may be considered, though they are used cautiously due to potential weakening of soft tissues.
Surgery
Surgical intervention is uncommon but may be necessary if shin splints are complicated by compartment syndrome.
A procedure called fasciotomy may be performed to relieve pressure within the affected compartments. Small incisions are made to release the fascia and restore normal blood flow. In acute cases, incisions may be left open temporarily before being closed once pressure normalizes.